

AS Patient Guidebook
What causes ankylosing spondylitis?
The cause of ankylosing spondylitis is not known, but there have been some important developments in our understanding of this condition over the last few years. What is known is that it is about three hundred times more common in people who inherit a certain white cell blood group numbered HLA B27 than in those who do not inherit this group. This white cell group is not related to the red cell blood groups, which are important in blood transfusions.
Who gets ankylosing spondylitis?
For a long time we have known that this back complaint "runs in families." The link with the white cell blood groups confirms this and will be discussed later in this booklet. Typically, the disease affects young men. However, we know that the illness occurs in women as well. Many people go through their lives with back complaints that are never really diagnosed as ankylosing spondylitis. We know now how important it is to recognize the condition early, because treatment is usually very helpful and the patient benefits from early diagnosis and, therefore, early treatment.
What is the difference between ankylosing spondylitis and other back ailments ?
Back troubles are some of the most common complaints seen in a doctor's office. In each year, 2% of a general practitioner's patients consult him with backache. Although most patients with back pain do not have ankylosing spondylitis, the doctor must recognize the different nature of the back problem in each patient. The most common back ailment is "back strain," which may occur at any age. A "slipped disk" is another example. In older patients degenerative, or wear-and-tear, problems commonly affect the back.
When a patient goes to the doctor with backache, the doctor must decide whether the problem is an inflammatory arthritis, that is, ankylosing spondylitis, or one of the common mechanical back problems. The treatment is different. The diagnosis is made by listening to the symptoms and examining the patient. The doctor may perform certain blood tests and examine X-ray films of the back. We will discuss these points separately.
What are the symptoms of ankylosing spondylitis?
Symptoms of ankylosing spondylitis that help distinguish it from mechanical causes of back pain are:
- slow (insidious) onset over weeks rather than hours
- age of onset around 20 or 25 years, rather than any age
- early morning stiffness and pain
- persistence for more than 3 months (rather than coming on in attacks)
- improvement with exercise, worse with rest (the opposite is true with mechanical problems)
Although we have been talking about a disease of the spine, pain is not always confined to the back. Some patients have chest pain which is worse on deep breathing, and felt around the ribs. This chest pain does not come from the heart but from the joints between the ribs and the backbone. Many patients complain of a shut-in feeling in the chest because it is difficult to move the ribs fully with deep breathing. However, the lungs can continue to work because the diaphragm is not affected.
When ankylosing spondylitis begins, it usually causes an ache felt in the buttocks and, possibly, down the backs of the thighs and in the lower part of the back. One side is commonly more painful than the other. This pain arises from the sacroiliac joints. The morning stiffness which is so characteristic of the condition wears off during the day. Many patients find that pain wakes them in the early morning, and if they get up and walk around, the discomfort settles. Patients may also experience the pain and stiffness after a prolonged period of sitting, as, for example, in a cinema or on a long car ride.
ankylosing spondylitis in its early stages may cause considerable pain, but effective treatment is available to relieve this, even though the discomfort is not always eliminated. Later the disease becomes much less active, or even totally inactive. The stiffness is rarely a handicap, provided that the spine is in a good position. Most patients with ankylosing spondylitis are able to carry on with their work and lead a normal life.
A few patients in the early stages of ankylosing spondylitis feel generally ill. In other words, they feel tired and miserable and may lose weight. It is not uncommon for them to be treated for depression. Some people may never have anything more than a series of mild aches and pains coming on and lasting for several months, never troubling them greatly. This seems to be more common in women with the disease. At this stage the disease can either clear up or it may go on to cause stiffening higher up the back, or in the neck.
Limb joints
Sometimes, either at the start or later, ankylosing spondylitis may affect joints other than in the spine. The shoulders, hips, knees, and ankles are the most commonly affected. The effect on these joints is similar to the effect on the spine,- there may well be a period of aching in the joint, perhaps with some swelling, but treatment relieves these symptoms and they settle down. Ultimately, there may be some restriction in the movement of the affected joints, but with proper treatment and active exercises from the start, the disability is slight. In particular, the hip joint must not be allowed to stiffen in a bent position.
Other trouble spots
Tender places may sometimes develop in bones that are not part of the spine. One of these is the heel bone, making it uncomfortable to stand on a hard floor, and another is the bone of the "seat" (ischium), making hard chairs unpleasant.
Does ankylosing spondylitis only affect the joints of the back and limbs ?
No. Other parts of the body may be affected. For example, attacks of inflammation of the eye occur in about 1 patient out of 7 sometime during their lives. These attacks are due to iritis, or inflammation in the colored part of the eye (the iris). A painful red eye should be reported to the doctor without delay, or permanent damage might occur. If the doctor is not available, then the patient should go directly to a hospital emergency room or ophthalmology department.
Other rare complications, happening in less than 1 patient in 100, may occur. These include problems in the heart, lungs, and central nervous system. Treatment is available for all of them. Patients with ankylosing spondylitis are not any more at risk of getting heart attacks, strokes, or cancer than the general population. Colitis, or inflammation of the bowel, is associated with ankylosing spondylitis in some patients, as is a skin condition called psoriasis.
Summary: ankylosing spondylitis
How is ankylosing spondylitis diagnosed?
Many patients have commented that their ankylosing spondylitis was not diagnosed until many months or years after their first symptoms began. There is no diagnostic test that the doctor can do at the onset of back pain, but the patient's symptoms, which differ from those of mechanical back pain, should alert the doctor to the diagnosis. Identification of the HLA B27 blood group alone would certainly not make the diagnosis, although it helps. The HLA B27 test is costly at the moment, but it will undoubtedly become a cheaper and more widely available test in time. At best, it may alert the doctor's attention to the fact that a patient may be developing ankylosing spondylitis.
The physical examination
The doctor will take a history and examine the back (looking for muscle spasm and noting posture and mobility) and then look at all the other parts of the body, searching for evidence of ankylosing spondylitis.
What tests will the doctor do?
The diagnosis of ankylosing spondylitis is confirmed from the X-ray. The characteristic changes are in the sacroiliac joints, but they may take some months to develop and may not be seen at the first consultation. The doctor will also probably test for anemia and do a test called the erythrocyte sedimentation rate (ESR), which tells how "active" the disease is.
What is the end result?
ankylosing spondylitis takes a different course in different people and no two cases are exactly the same. The symptoms may come and go over long periods, but in the end ankylosing spondylitis almost always settles down. The lumbar spine usually becomes stiff, and the upper part of the back and the neck can stiffen as well.
It is for this reason that it is so important for patients to maintain a good posture. The worst disability that can follow ankylosing spondylitis is fixation of your back in a bent or stooped position. This used to be common but is now prevented by early diagnosis and treatment. Not every patient with ankylosing spondylitis who maintains a good posture and follows an exercise program will return to normal, but serious deformities can be prevented by these measures. The patient who stiffens in a bent position has difficulty in looking straight in front and compensates by straining other muscles and joints, which gives rise to more pain.
People with ankylosing spondylitis can often be acutely aware of their own appearance and how they might look different from other people. Most patients can come to terms with the problem, even though this may be difficult.
What is the treatment?
There is no cure for ankylosing spondylitis. The doctor aims to relieve the symptoms, improve spinal mobility where this has been lost, and allow you to follow a normal occupational and social life. Although with increasing age the disease tends to become less active, you should realize that the treatment must continue more or less forever. In particular, you must pay continuous attention to adequate posture, mobility, and exercises.
The patient and doctor alike play an active role in the management of this condition, usually with the help of a physical therapist. Occasional visits to the doctor will ensure that an adequate management program is being followed. Although the treatment section of this handbook is divided into separate sections for drug treatment, posture, physical therapy, and exercises, these aspects of treatment will vary with the individual patient.
As part of the treatment of ankylosing spondylitis it is important that you, as the patient, take care of your health and posture. This includes not allowing yourself to become overweight or overtired from working overtime or taking on too many commitments. The motto for treatment which all patients should learn like a catechism is:
It is the doctor's job to relieve pain and the patient's job to keep exercising and maintain a good posture.
Your general health
At times when ankylosing spondylitis is active, your health as a whole suffers; you may lose weight, get unusually tired, even depressed, or become anemic. At such times in addition to treatment for the back, you will need extra rest and a good nourishing diet.
A good diet in this case is one giving you at least two helpings of protein food each day - meat or fish. Fruit and vegetables are sources of vitamins, and a pint of milk daily will give you a sufficient supply of calcium. If necessary, your doctor may give you iron tablets for anemia.
Drug treatment
Although the disease cannot be cured, most of the trouble it can cause can be helped or prevented. In the first instance, the doctor will prescribe for you a drug that relieves pain (analgesic) and inflammation. There is a wide range of drugs that will reduce or abolish the pain and give you a good night's sleep and sufficient freedom from pain to take part in an active exercise program.
Principles of treatment
Many patients find that they require continuous treatment on a small maintenance. dose of their drug. Some of the newer tablets are manufactured to remain effective within the patient throughout the night and into the first part of the day. If you cannot find a suitable tablet to last throughout the night, suppositories may be used. It is not necessary to give drugs by injection. None of the drugs used for ankylosing spondylitis is habit-forming (i.e. patients don't get addicted to them).
Posture
Since ankylosing spondylitis left untreated causes increasing flexion of the spine (the patient becomes progressively more stooped), every endeavor must be directed toward keeping as straight and erect as possible. It is rare for the spine to stiffen completely but, in case this might happen, you should do everything to ensure that it at least stiffens in an erect rather than a bent position.
Sitting posture. To maintain good posture while sitting, use a chair with a firm seat, straight back, and armrests. Firm padding on the seat and back will make you more comfortable. The seat of the chair should not be too long from front to back because this might make it difficult to place your lower spine into the base of the back of the chair. Don't sit for long in low soft chairs as this will result in bad posture and increased pain.
At work. Pay special attention to the position of your back when at work, so that you do not have to stoop. If you sit at a desk or bench, see that your seat is at the proper height and do not sit in one position for too long without moving your back. A job that allows a variety of movements - sitting, standing, and walking - is ideal. The most unsuitable work is that in which you stoop or crouch over a bench for hours at a time. If you have a heavy or tiring job, do not tackle other activities at home or elsewhere until you have had a break, lying flat for a time if necessary. It may also help if you can lie flat for 20 minutes at midday. At such times try to lie for part of the time face downward.
Car driving. If you ever have to make a long car journey, it is important to stop for 5 minutes every hour or so and get out of the car for a stretch. Pain and stiffness can distract your attention, which is so vital for your safety if you are driving.
Many patients with stiffness of the neck and other parts of their spine have difficulty backing into parking spaces or a garage because they cannot turn easily to look behind them. It is possible to fit special mirrors onto your car to help you. You should practice backing up using this new technique in an open area with some light wooden obstacles to act as markers. (A piece of broom handle stuck into the ground could serve this purpose.) Head rests are advised so that sudden deceleration injuries to the neck can be avoided. The stiff neck of an ankylosing spondylitis patient is more easily hurt than a normal neck. Disabled drivers' permits may be appropriate if you can't walk very far, but this is a rare problem in ankylosing spondylitis.
Rest. If ankylosing spondylitis is very active and the stiffness very troublesome, a spell off from work or in the hospital may be necessary. This does not mean resting immobile, for this might hasten the stiffening of the spine. So even a spell of rest from work means that you will be encouraged to do exercises for your back and chest and limbs to keep them supple, When you are lying in bed it is important that you should be quite flat on your back and, also, some of the time you should practice lying on your face. "Prone lying," as it is called, is best done for 20 minutes before rising in the mornings, and 20 minutes before going to bed at night.
At first you may not be able to tolerate more than 5 minutes of prone lying at a time, or may even need a pillow under your chest, but with practice, as the spine relaxes, it will become easier. If you make a habit of this it will help prevent your back and hips from becoming bent. Although this period of prone lying may not be practical every day, at least some time devoted to it is better than nothing at all.
Your bed. The bed you sleep on should be firm and without sag. If you have a soft or saggy mattress, get a suitable board to put between the mattress and the bed frame. A sheet of plywood or chipboard 2' x 5' x 1/2" is ideal. You will find that this bed is more comfortable to lie on than one that is too yielding. Afterward, when the painful active phase of spondylitis is past, it is important to keep a firm bed to prevent any tendency for spinal curvature to develop later.
Corsets and braces. In general, corsets and braces are of no value whatsoever, and indeed can make ankylosing spondylitis worse. It is better to develop your own muscles and retain a good posture by natural means. Very occasionally some form of bracing may be necessary, for example, after a back injury, but this decision should be made by a doctor who is experienced in treating patients with ankylosing spondylitis.
Physical therapy
Desk Exercises html version or the PowerPoint version (848384 kb)
by Dr. Ellyn Robinson, CSCD*D, CPT. Thank you very much.
Probably, at some time, you will receive treatment from a physical therapist, and you should learn an exercise routine which you can do every day. The exercises will be tailored to your individual requirements and, for this purpose, you should attend a Physical Therapy Department for one or two sessions to learn your exercises. The physical therapist, however, may require a referral from a doctor, so in the first place you must approach your doctor.
Until you have a set of exercises of your own you should make a start right away by doing daily exercises. Some of these are shown below. You may not be able to do all of the exercises, but do what you can. Their purpose is to make you conscious of your posture, especially the position of your back, and to encourage free movement of certain joints, particularly shoulders and hips. It is important to keep your muscles strong, because reduced movement, even for a short time, allows them to become weaker and it may take a long time to build them up again.
Sporting activities. Many patients ask what sporting activities are suitable for them and the most ideal one is swimming, since it uses all the muscles and joints without jarring them, Regular swimming is something the whole family can enjoy.
Some young patients enjoy cross-country running or tennis. Contact sports are not ideal because the joints can get injured. Even golf has its drawbacks, because patients may spend long periods practicing putting, during which the spine is in continued flexion. Badminton can be beneficial and also squash when the disease is going through remission. Basketball and volleyball are excellent as they combine movement with stretching and jumping.
However, not all patients tolerate weight-bearing and jarring activities. Bicycling is a very beneficial form of exercise because it helps keep the joints active and gives more strength in the legs. It is also a good breathing exercise and helps the rib cage to continue in its expansion, provided that the handlebars are adjusted properly so that the rider is sitting tall.
Physical therapy: General reminders
Heat. In its various forms heat will help to relieve the pain and stiffness, A hot bath before retiring, or a hot water bottle or electric blanket in your bed may be quite enough. It is not necessary to use special lamps.
Surgery. Surgery has only a small place in the treatment of ankylosing spondylitis. It is used in restoring movement to damaged hip joints (arthroplasty) and, rarely, in straightening the back or neck in patients who have become so bent over that they cannot look forward and are having difficulty in crossing the road.
Folk remedies. Do not be beguiled into buying expensive treatments whose effectiveness has not been medically proved. For patients with stiff necks, manipulation can be dangerous.
 To understand the disease, we can take a closer look at the spine. The spine
is made up of 24 vertebrae and 110 joints. The three main sections of
vertebrae-the cervical, thoracic, and lumbar-differ somewhat in their
form and their natural curvature. The cervical, or neck, vertebrae are
the most mobile. In the thoracic section, each vertebra has a rib attached
by joints on each side of it.
To understand the disease, we can take a closer look at the spine. The spine
is made up of 24 vertebrae and 110 joints. The three main sections of
vertebrae-the cervical, thoracic, and lumbar-differ somewhat in their
form and their natural curvature. The cervical, or neck, vertebrae are
the most mobile. In the thoracic section, each vertebra has a rib attached
by joints on each side of it.
Above, the lumbar section is the sacrum, which sits like a keystone
in the ring of bone which forms the pelvis. The joints between the sides
of the sacrum and the pelvis, called the sacroiliac joints, are the
starting points for ankylosing spondylitis.
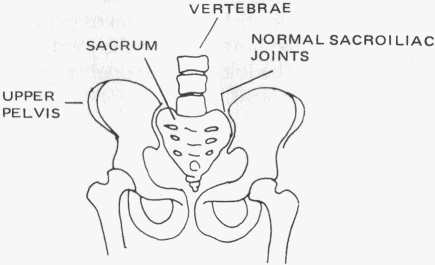
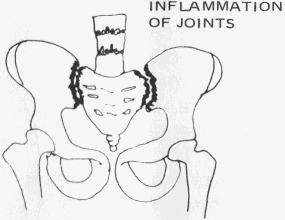 In the early stages of the disease, changes begin to take place in the sacrum
and upper pelvis. Here we also see evidence of changes in the joints between
the vertebrae.
In the early stages of the disease, changes begin to take place in the sacrum
and upper pelvis. Here we also see evidence of changes in the joints between
the vertebrae.
 In
the advanced stage, the sacroiliac joints are fused, and the joints between
the vertebrae have also grown together by boney changes. This produces
the effect sometimes known as "bamboo spine."
In
the advanced stage, the sacroiliac joints are fused, and the joints between
the vertebrae have also grown together by boney changes. This produces
the effect sometimes known as "bamboo spine."
Daily exercises
1. Standing with your heels and seat against a wall and keeping your chin in, push your head back toward the wall and keep it back for the count of 5, then relax. Repeat 10 times.

2. Sit on a firm chair, put your right hand across your chest and hold the side of the chair. Stretch your left arm out in front of you and then twist to the left, taking the arm horizontally as far behind you as possible, turning your head to look over the left shoulder. Hold this position, then push and turn a little further, hold that position and then return to facing forward. Repeat 3 times with each arm.

3a. Sit with your shoulders relaxed and chin drawn in, looking straight ahead. Bend your head sideways to bring your right ear toward your right shoulder, hold it there, make sure your shoulder muscles are still relaxed and bend a bit further, then return to straight. (As you do the side bending, the profile of your nose should remain in the same place, to make sure you don't turn your head.) Repeat to each side twice.

3b. Now tip your head back, looking up the wall and along the ceiling and bring it back to straight. Repeat.
Change to tipping your head forward as far as possible to get your chin touching your neck, and return to straight with chin pulled in. Repeat.
4. Still lying on your back with knees bent up, lift up your hips, so your seat is off the floor and there is a straight line from shoulder to knees. Hold for the count of 5, and lower. Repeat 5 times.

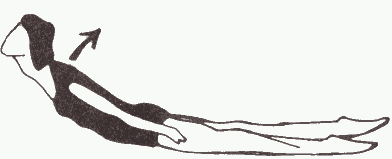
5. Lie on your front, head turned to one side, hands by your sides. (If necessary, you may put a pillow under your chest, but not your waist, in order to get comfortable.)
(a) Raise one leg off the ground, keeping your knee straight, 5 times each leg, making sure your thigh comes off the ground.

(b) Raise your head and shoulders off the ground as high as you can 10 times.
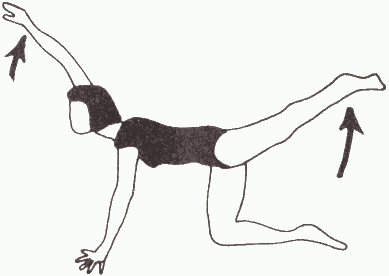
6. Kneeling on the floor on all fours, stretch the opposite arm and leg out parallel with the floor and hold for the count of 10. Lower and then repeat with other arm and leg. Repeat 5 times each side.
Breathing exercises
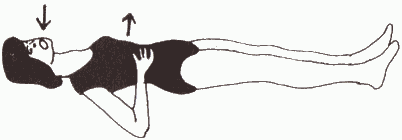
7. Lie on your back, legs straight.
a. Put your hands on your ribs at the sides of chest. Breathe in deeply through your nose and out through your mouth, pushing your ribs out against your hands as you breathe in. Repeat 10 times. (Remember, it is as important to breathe out fully as it is to breathe in deeply.)
b. Put your hands on the upper part of the front of your chest. Breathe in deeply through your nose and then breathe out as far as you can through your mouth. Push your ribs up against your hands as you breathe in. Repeat 10 times.
Other topics
ankylosing spondylitis in the family
In most populations of European origin, ankylosing spondylitis is virtually confined to those who inherit the white cell group HLA B27. This group occurs in 7% to 1 0% of the population. This means that virtually all people with ankylosing spondylitis will have this particular blood group. However, it is very important to note that the reverse is not true. There are far more people with the blood group who never get ankylosing spondylitis than those who do get it. Even in families where one member has ankylosing spondylitis, a brother or sister can have the blood group and never get the disease.
The present evidence suggests that about 20% of individuals with HLA B27 will get ankylosing spondylitis. Since HLA B27 is present in 7% to 10% of the population, a little over 1 in 100 individuals will develop the disease. Most will never have it diagnosed, as it will be in a mild form.
The chances of your children developing ankylosing spondylitis are quite low, not more than 5 in 100, compared with 95 out of 100 chances of producing normal healthy children. Even of this 5% who get the disease, probably only I in 5 will get the condition severely enough to interfere with a normal life. Parents with ankylosing spondylitis sometimes ask if they should have their children bloodgrouped to see which ones have HLA B27. The answer at present is that this should not be done since there is no way of knowing which child with this blood group would get the disease. If there comes a time when we are able to prevent ankylosing spondylitis, then it would be important to find out which children carried the HLA B27 blood group, so that they could be protected from the disease.
ankylosing spondylitis in men vs. women
Until recently ankylosing spondylitis was considered to be much more common in men than women. We now have evidence to suggest that women, too, frequently develop the disease. It does seem that some women have a very mild form of the condition which may not, in fact, be easy to detect.
Pregnancy and sex
ankylosing spondylitis does not usually interfere with normal lovemaking, unless the hips are affected, in which case the modern operation of hip arthroplasty may help considerably in freeing hip movement. The Arthritis Foundation has published a booklet entitled "Living & Loving: Information About Sex" which is obtainable by writing to The Arthritis Foundation, 1314 Spring Street NW, Atlanta, Georgia 30309.
Pregnancy in women with ankylosing spondylitis holds no particular hazard for the mother and baby, but in contrast with some other forms of rheumatism the spondylitis does not die down during pregnancy. The babies are usually born by the normal route, but occasionally it is necessary to have a Caesarean operation if the hip joints become very rigid.
Postscript
ankylosing spondylitis is not a sentence to life-long unemployment. Experience says that patients with ankylosing spondylitis are capable of doing a wide variety of jobs, whether intellectual, semi-skilled, or even manual. Thus, among this special group of people there are examples of patients having physically stressful occupations, such as carpenters and builders, and there are also patients who have pursued outstandingly successful professional and business careers.
APPENDIX: Case Histories
ankylosing spondylitis is a very variable disease. The typical course described in this pamphlet does not occur in every patient and, for this reason, a few case histories are presented below.
24-year old man whose disease started in childhood
At the age of 1 this patient developed a swollen right knee which did not respond to aspirin treatment. He was seen at his local hospital and the leg was put into a plaster of Paris splint for 6 weeks. The knee was very stiff after this but the swelling had settled, After 3 months of physical therapy the knee had returned to normal. A similar episode occurred when the patient was 14 years old, and the knee settled, as on the first occasion.
At the age of 21 he began to get pain in the buttocks and the top of his legs, which was thought to be lumbago. He found that aspirin had no effect on the pain, which would wake him at night. He was so stiff in the mornings that he had to wake himself an hour earlier to loosen up so that he could get to work on time. He decided to see an osteopath, who manipulated his spine on three occasions. The pain seemed to be worse after the manipulations, for 2 or 3 days, so he stopped going.
At the age of 24 he was referred to the hospital, where a diagnosis of ankylosing spondylitis was made. At the time of his referral he had been getting bouts of low back pain waking him at night for about 4 months. He was demoralized and had changed his job from working in a warehouse, doing heavy lifting, to a clerical one. The change had not helped his back. He responded well to appropriate drug treatment and physical therapy. The nature of his disease was explained to him and he felt much less depressed about it.
Comment: This man's disease began in childhood but it was not possible to make a diagnosis at that stage. Osteopathic manipulation made his symptoms worse, whereas controlled exercise, as instructed in the physical therapy department, proved to be useful.
48-year old man whose disease did not go into remission
This patient first noticed low back pain while he was in the Army at the age of 21. He would awaken with severe pain and stiffness at 5 a.m. His disease was not recognized at that time and it was felt that he was trying to get out of his National Service.
While on leave his parents took him to see an orthopedic surgeon, who found that he had an elevated ESR. The diagnosis of ankylosing spondylitis was suspected at that time, although his X-rays did not show any abnormality. He was discharged from the Army and got a job as a salesman. The back pain persisted, although painkillers did dull the discomfort. He never seemed to get periods of relief from the pain. Gradually the pain caused him to adopt a stooped posture, which has never improved in spite of exercises. He did find that when phenylbutazone first became available the pain was much easier to tolerate, and his stoop never progressed after that time.
Comment: This patient is unusual in that his ankylosing spondylitis has not gone into periods of remission, but this is known to occur in a few patients. His back deformity was, however, halted once he was given an effective drug.
31-year-old woman whose disease was reactivated after an injury
The patient developed ankylosing spondylitis at the age of 19, but after 3 years she was free of symptoms. At the age of 31 she was "shaken up" in a car accident; no bones were broken but she was bruised around the face, chest, and thighs. Two days after the accident she developed acute pain in the thoracic spine, which was worse on breathing. She had to be given large doses of painkilling drugs to settle the pain. The ankylosing spondylitis became reactivated in the thoracic spine and took 4 months to settle. Her chest expansion, which had previously been normal, was reduced to less than half.
73-year-old woman with advanced ankylosing spondylitis and no history of backache
This elderly patient was knocked over by a passing car while she was crossing the road. In the emergency room of the local hospital she was found to have fractured her lumbar spine, which was rigid from ankylosing spondylitis. She denies having any back pain during her life.
Comment: This-is exceptionally rare but does illustrate the fact that X-rays may look impressive, but the symptoms don't always match them. The reverse is also true, namely, a great deal of pain may not be accompanied by any X-ray features. As mentioned before, ankylosing spondylitis seems to run a less painful course in women than in men. Men also have their ankylosing spondylitis diagnosed much earlier than women, on the whole.
The ankylosing Spondylitis Association wishes to thank the British National ankylosing Spondylitis Society for permission to reprint and distribute this booklet in America.
The ankylosing Spondylitis Association is grateful to CIBA-GEIGY Corporation, Pharmaceuticals Division, for their help in producing this booklet.